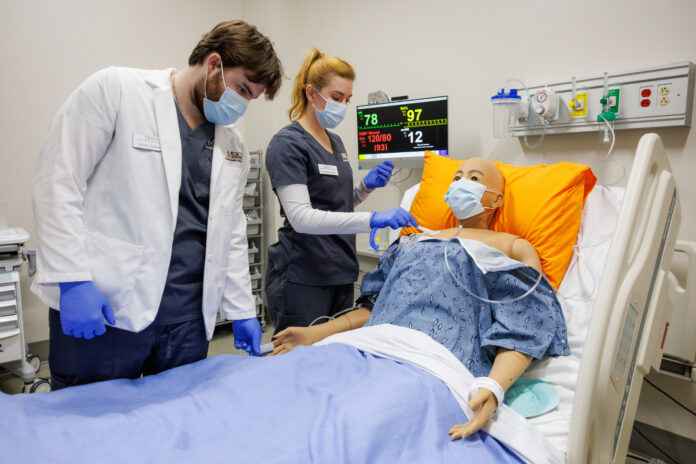
Standing outside the door to a simulated hospital room, two Georgia Baptist College of Nursing of Mercer University undergraduate students are briefed on the patient inside. A male, born in 1965 and admitted with pneumonia, needs a sterile central line dressing change and is reporting a cough and shortness of breath.
The students enter the room and begin checking on the patient, represented by a full-body simulator called a high-fidelity manikin, which mimics the human body and responds to interventions accordingly. Meanwhile, Dr. Jennifer Bartlett, professor and associate dean of nursing for the Macon campus, sits behind one-way glass, controlling the manikin, which blinks, breathes and vocalizes. She’s also observing the students.
The students sanitize their hands and put on gloves. They ask the patient if it’s OK to sit him up in bed.
“Yes. I can’t breathe,” Dr. Bartlett says in a low, scratchy voice, speaking into a microphone. For the students in the patient’s room, the voice comes from the manikin. The patient coughs, and the students begin performing their assessment.
Dr. Bartlett notes the low oxygen saturation level on a monitor in the patient’s room. The students should be giving the patient oxygen, but they’re not, so she lowers it even more. The students notice and start connecting the patient to oxygen. While they’re working to stabilize and assess the patient and perform the required dressing change, the patient asks for a cigarette.
“They’re trying to do the skill and are interrupted by the patient,” Dr. Bartlett says to an observer in the room with her.
Practicing their skills with interruptions helps increase the students’ cognitive load and teaches them to perform under stress, she said.
The whole simulation lasts just 15-20 minutes. By the end, the students have changed the patient’s central line dressing using sterile technique and addressed his pain. After the simulation, the students watch a video recorded during the exercise and are guided through a semi-structured debrief designed to solidify their learning.

“We tend to use simulation as formative, meaning it’s really all about the learning, providing a safe and brave space for them to have these experiences,” Dr. Bartlett said. “We align the placement of the simulations with what’s going on in their coursework. We’re really able to reinforce what they’re doing in the classroom through simulation.”
A key aspect of a Mercer nursing education is giving students of all levels a place to practice the skills they learn in the classroom in a controlled space before clinical rotations. In addition to simulations with high-fidelity manikins, the College of Nursing offers skills labs using realistic replicas of body parts known as task trainers; real-life simulations using mixed reality, which is similar to virtual reality; high-tech teaching equipment; and in-person scenarios with actors known as standardized patients.
Each method aims to build students’ confidence and competence, said Dr. Bartlett, who is a Certified Healthcare Simulation Educator with extensive experience in the development, implementation and evaluation of nursing simulation. She also has served as a simulation consultant nationally and internationally.
“Students develop competence in their assessment skills, their situational awareness, their emotional intelligence, their ability to collaborate, their ability to lead a team, and their ability to perform skills within a specific context,” she said. “All of that, and the cognitive load and cognitive stacking that occurs when multiple things are going on, increases their competence.
“Because of these simulations, and especially in the debrief, we see their confidence also increases. They’re more willing to step into a situation in the real world. They have a script. They feel like they’ve been in this situation clinically even though it was just a simulation.”
Traditional Prelicensure BSN
Students pursuing a traditional prelicensure Bachelor of Science in Nursing degree in Macon and Atlanta practice in skills labs and simulations with high-fidelity manikins.

During their first semester of nursing school, students participate in skills labs as part of their fundamentals and health assessment courses, said Dr. Emma El-Shami, clinical assistant professor in Atlanta.
In the fundamentals course, students learn many skills, including how to properly wash their hands, put on personal protective equipment, use assistive devices like canes and wheelchairs, and safely transfer and position patients. They also use task trainers to learn how to do a central line dressing change, place a urinary catheter and care for a wound, she said.
In the health assessment class, students learn how to do a head-to-toe physical assessment of a patient. Each week focuses on a different body system, and at the end, students put it all together in a complete assessment, Dr. El-Shami said.
Simulations with the high-fidelity manikins start off basic, with objectives including taking vitals and caring for a wound, she said. As students advance in their second year, the simulations become more complicated. They may have to do a sepsis protocol, blood transfusion, respond to a stroke or deal with an end-of-life scenario.
“Nursing is such a hands-on profession that you really can’t learn it unless you’re doing it,” Dr. El-Shami said. “It’s one thing to read about how to take a blood pressure, but you won’t really understand how to take a blood pressure until you’re actually doing it and have to listen to hear someone’s diastolic and systolic blood pressure. It’s the same thing listening to heart sounds, lung sounds, bowel sounds, anytime we’re using our stethoscope and equipment.
“Most everything that we do in the hospital is tactile. For nursing students, it really is the best way for them to learn.”

Nicole Russo, a first-year nursing student in Atlanta, said the fundamentals and health assessment labs made her more confident when she went into clinicals.
“We perform head-to-toe assessments, not to the extent that we learned in lab, but we perform them all the time just when we walk in the room,” she said.
Meanwhile, she said the simulations with the high-fidelity manikins developed her critical thinking and helped her learn how to think on her feet.
“It’s hard, but if we don’t learn it now, we’re going to be learning it at the bedside, and it’s better to make the mistakes and learn from them now rather doing it to the real person,” she said.
Wesley Adams, a first-year nursing student in Macon, said the simulations also teach teamwork, not only with the other students in the room but with other medical professionals, played by their professors, such as the charge nurse and secretary.
“Our professors do a very good job of making it a real-world scenario,” he said.
Accelerated Bachelor of Science in Nursing
Students in the Accelerated Bachelor of Science in Nursing program learn using task trainers and mixed-reality simulations in addition to the high-fidelity manikin simulations.
Task trainers allow students to home in on a particular task without having to use an entire complex manikin, said Dr. Tabatha Anderson, clinical assistant professor and director of the ABSN program, which is primarily taught online with labs at a campus in Cobb County.
For example, students use a task trainer that looks like an arm to learn how to start an IV. The arm has veins in it and is hooked up to simulated blood.

“When you’re starting an IV on a person and you put the IV in, you see a little bit of blood come back in the IV catheter so that you know you’re in the vein,” she said. “These are arms that simulate an actual IV start that can give a student a more realistic experience to better prepare them for performing skills in the clinical setting.”
In mixed reality, students wear a headset that puts them in a virtual scenario taking place in their environment. For example, a student can be standing next to a bed in the lab and see a virtual patient sitting on the bed. The student can then interact with the patient in this mixed-reality environment, Dr. Anderson said.
Mixed-reality scenarios are best for the student to practice interacting with patients and their family, she said. In one scenario, a child is suspected of being abused. In this simulation, the student can observe bruising on the virtual child and question the virtual mother, who responds based on what she is being asked.
“There are some things within nursing that are incredibly important that the students experience, and one of those things is emotionally difficult situations or the psycho-social interactions with patients and their families,” Dr. Anderson said. “This is a way we can interact and put the student in that situation, so all students get those valuable experiences and support within a safe learning environment.”
ABSN student Kevin Hazzard was surprised at how realistic the mixed-reality simulations were. As a former paramedic, he already had experience in high-stakes situations and found typical educational scenarios stilted.
“Everybody knows it’s a scenario, and it makes it difficult to get into it because the realism factor isn’t quite there,” he said. “With this, it very much is.”
He recalled a mixed-reality scenario in which he was treating a patient in alcohol withdrawal. The patient was agitated with vital signs all over the place and was borderline violent, he said.
“Anyone walking into that room immediately realizes if you’re dealing with an agitated patient, you don’t have time to take your focus off them and do other things,” he said. “You have to continually work to sort of calm them down and gain their trust so that you can get their cooperation, so you can do what you need to do, which is ultimately help them, but they’re not really in a condition to either understand or necessarily care about that in the moment.
“That sort of realism in training, I think, is invaluable,” he said. “It’s one thing to know the information. It’s another thing to put it into practice, and a program like this really allows you to put it into practice because it forces you to do the right thing quickly and in a sequence that makes sense to this patient. Otherwise, the situation is going to escalate.”
Graduate programs
The College of Nursing’s graduate programs in Atlanta offer tailored lab experiences based on the students’ focus areas.

Acute care students use high-fidelity manikins, task trainers and specialized equipment that allow them to practice skills they would use on patients, said Dr. Humberto Reinoso, associate professor and nurse practitioner coordinator.
One example of this specialized equipment is SonoSim, a probe and computer program that teaches students how to perform an ultrasound. To use it, a sensor, which connects to a probe, is placed on a manikin. Then, the student can use the probe and see the simulated ultrasound results on a computer.
“They’ll be able to see some pathology on the manikin without having to wait for that particular scenario to present itself in the clinical setting,” Dr. Reinoso said. “The benefit of that is when they do get a patient in the clinical setting, let’s say they need to do a FAST (Focused Assessment with Sonography for Trauma) exam or they need to look at a gallbladder or whatnot, they have the dexterity, and they’re able to identify where to place the probe and so forth.”
Students pursuing primary care or psychiatric-mental health care run through simulations with standardized patients. Faculty send a scenario to the actor, who learns the case.
“On the day of the intensive, the student will approach that patient like a clinical patient. We simulate the room, their interaction, their introduction, and then we have that evolving case,” Dr. Reinoso said. “Students ask the questions, and they get the answer. We have preprinted diagnostics that they’ll be able to request at that point in time.
“It’s an evolving case that the faculty are there to supervise, so the student gets that clinical experience in a controlled environment, and then faculty are able to evaluate their performance, and then we are able to give them feedback.”
Because faculty in the program are also practicing nurse practitioners, they have students simulate what they’re seeing in practice to give that real-world experience, he said.
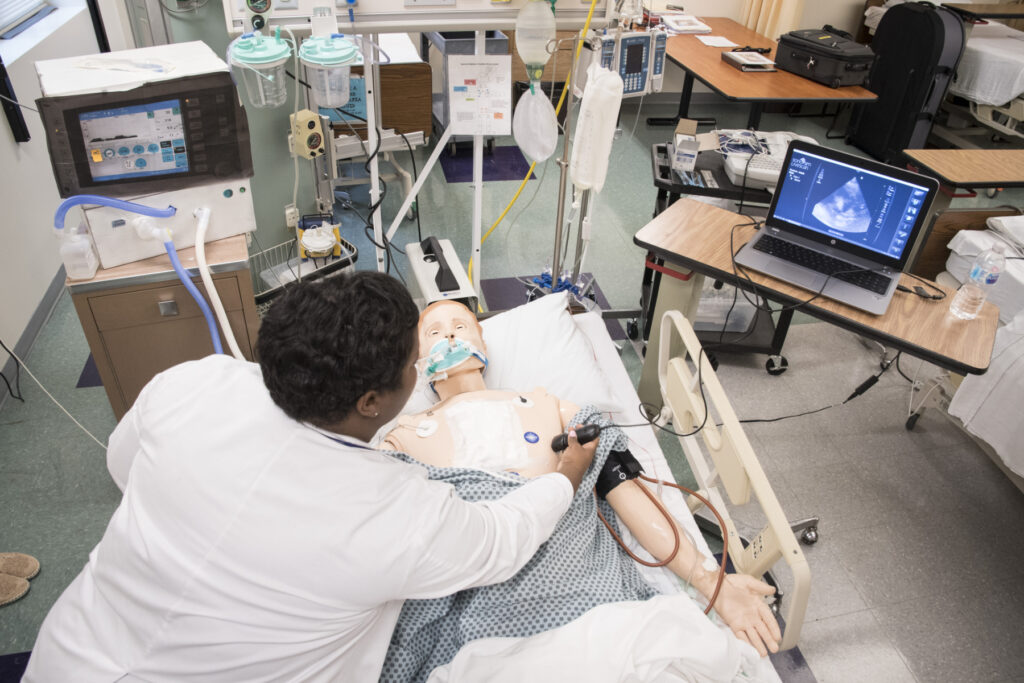
Mira Mehta, a critical care nurse who is pursuing a Master of Science in Nursing on the adult-gerontology acute care nurse practitioner track, said learning with the SonoSim made her feel prepared for her clinical experience. Working with the standardized patients was her best learning experience, followed by using the high-fidelity manikin, she said.
“I had a (standardized) patient who came in with serotonin syndrome. You don’t know that going in, so you go in and you assess the patient. You talk to them,” she said. “I don’t know how (the actor) did it, but she actually looked diaphoretic. She looked sweaty. I don’t know how she was acting that out, but she did a really good job, and that was one of the key things that I noticed pointing me toward the diagnosis.”
She said she appreciated the experience of various simulations in a structured environment, where it was OK to make mistakes and learn from them.
“Truly, I think that was probably the most beneficial time because you also have an instructor there to critique you and help you understand where you can be better,” she said.