Mercer University professors Caroline Anglim, Ph.D., and Paul Lewis, Ph.D., M.Div., have received a $60,000 Faith and Health Campus Grant from Interfaith America to expand both academic and public understanding of how faith, spirituality and health intersect.
The initiative will aim to advance the concept of religion as a social determinant of dying well in the American health care system and include several components including curricular development, community partnerships and research. The research component will analyze how religion factors into the experience of dying and explore how religious and health care leaders might work together to better support dying patients and their families.
The project grew out of an existing initiative within the School of Medicine’s bioethics and medical humanities department. In that program, hospital chaplains work with medical students to develop religious literacy and apply those skills during standardized patient encounters. Standardized patients are trained individuals who portray specific clinical scenarios. This prepares medical students to help support patients who are dealing with existential crises in the context of their medical crises.

Dr. Anglim, assistant professor of bioethics and medical humanities at the School of Medicine, said, “Thanks to our community medicine department and population health rotations, our students walk away from their medical education with a clear idea of social determinants of health. This project will help them understand how religion also operates as a determinant of health by informing medical decision-making and health behaviors.”
Dr. Lewis, professor and chair of the department of religion in the College of Liberal Arts and Sciences, was invited to join the project because he teaches the award-winning course on death and dying.
“Traditionally, medical schools train doctors to fix parts and not people. You spend so much time on the science part of it, the human side can get lost,” said Dr. Lewis. “This program helps students understand the importance of palliative care where the care team says, ‘We’re not going to abandon you even if we can’t cure you.’”

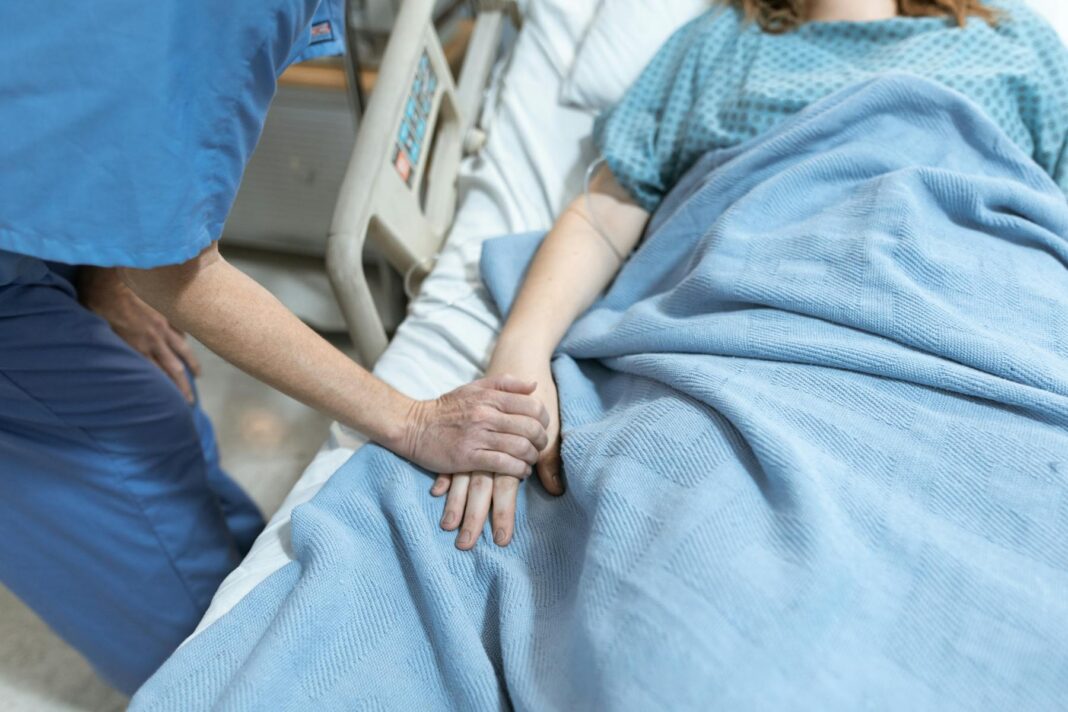
The grant will focus on palliative and hospice medicine, where the goal is not always to cure but to provide comfort and support at the end of life. Its research, education and public programming will explore how religious communities prepare for and respond to death, how spirituality shapes mental health during this time, and what religious resources may improve the experience of dying. It will also examine how leaders in faith communities and health care can work together to better support patients and their families.
“Medical students read lots of scientific articles but don’t always get the opportunity to engage with complex, philosophical ideas in a sustained way,” said Dr. Anglim. “Our goal is to train them to approach the experience of illness and treatment of illness in a different way, not just as fixing the medical problem.”
In the first project phase, undergraduate students will begin their research projects through the Mercer Undergraduate Research Scholar Training Initiative, and medical students will conduct research under the grant through the Summer Scholars Program. The second phase will begin in the fall when students will read books and texts, as part of a reading group, on death and dying from perspectives of bioethics, medical humanities, anthropology and more.
“This project is another way that Mercer can honor its religious heritage,” said Dr. Lewis. “Researching religion as a social determinant of health is a way of being faithful to that heritage and doing it in a way that’s consistent with freedom of inquiry.”
In addition to the student initiatives, Dr. Anglim and Dr. Lewis will implement a series of initiatives to integrate interfaith learning into clinical and community health settings over the next two years. They will also join a national community of practice and engage in sector-wide learning with peers in public health, medicine, nursing and related fields. Grantees are invited to attend Interfaith America’s 2026 Interfaith Leadership Summit in Chicago and participate in a dedicated Faith and Health Educator Track.
The 2026 Faith and Health Campus Grant funding supports innovative work at the intersection of religious diversity and health and is part of Interfaith America’s three-year Faith in Health Professions project funded by the John Templeton Foundation. The Faith and Health Campus Grants and Faith in Health Professions Project support Interfaith America’s mission by promoting religious pluralism across the health landscape through curricular and co-curricular learning, research and robust community partnerships.
About Interfaith America
Interfaith America was founded in 2002 based on the idea that religious differences should serve as a bridge of cooperation rather than a barrier of division. Since that time, Interfaith America has evolved from a small Chicago-based nonprofit to the nation’s premier interfaith organization. Led by Founder and President Eboo Patel, Interfaith America inspires, equips, and connects leaders and institutions to unlock the potential of America’s religious diversity. Utilizing a research-backed approach, Interfaith America works across higher education, racial equity, health, the workplace, bridge building, democracy and technology. To learn more, visit InterfaithAmerica.org.
About Mercer University School of Medicine (Macon, Savannah, Columbus and Valdosta)
Mercer University’s School of Medicine was established in 1982 to educate physicians and health professionals to meet the primary care and health care needs of rural and medically underserved areas of Georgia. Today, more than 60% of graduates currently practice in the state of Georgia, and of those, more than 80% are practicing in rural or medically underserved areas of Georgia. Mercer medical students benefit from a problem-based medical education program that provides early patient care experiences. Such an academic environment fosters the early development of clinical problem-solving and instills in each student an awareness of the place of the basic medical sciences in medical practice. The School opened additional four-year M.D. campuses in Savannah in 2008 and in Columbus in 2021, and a clinical campus in Valdosta in 2024. Following their second year, students participate in core clinical clerkships at the School’s primary teaching hospitals: Atrium Health Navicent The Medical Center and Piedmont Macon Medical Center in Macon; Memorial Health University Medical Center in Savannah; Piedmont Columbus Regional Hospital and St. Francis Hospital in Columbus; and SGMC Health in Valdosta. The School also offers master’s degrees in preclinical sciences and family therapy and Ph.Ds. in biomedical sciences and rural health sciences.