By Marlene Goldman
It all started with a toothache. Then came a root canal and a prescription for pain that sent the 30-something pharmaceutical sales rep into the downward spiral of addiction. He soon became a “seeker” and used his extensive network of physicians, pharmacists and Internet sales to feed a 30-hydrocodone-a-day habit. As his insatiable craving grew, his life nosedived. He was broke and close to losing everything when he finally sought help.
His was a classic addiction story, but he survived through medication-assisted treatment (MAT) and counseling. Many Americans aren’t so lucky.
The United States has the world’s highest rate of opioid addiction and mortality.
Over the past 20 years, the number of opioid prescriptions has quadrupled. The U.S. represents less than 5 percent of the world’s population but takes more than 99 percent of prescribed hydrocodone. Opioid overdoses are the No. 1 cause of premature deaths of males — more than traffic accidents, more than gunshot wounds. Opioid addiction is the No. 1 reason for incarceration.
“It’s worse than the AIDS epidemic,” said Kevin Murnane, Ph.D., assistant professor of pharmaceutical sciences in Mercer’s College of Pharmacy.
Though prescribing of opiate pain medication is beginning to level off or even decline slightly in some areas, use of heroin and illicit synthetic opiates and deaths due to accidental overdoses continue to increase sharply. Heroin is now commonly contaminated with fentanyl or carfentanyl — superpotent narcotics that dramatically increase the risk of fatal overdose. Emergency responders often must give multiple doses of naloxone to revive people who have overdosed.

Georgia ranks in the top 12 states in terms of drug abuse. Opioid-related deaths in this state have increased more than tenfold over the past 15 years compared to a fourfold increase across the rest of the nation.
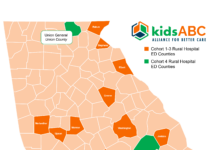
The burden of the epidemic is especially heavy in Georgia’s rural and underserved areas — 35 percent of Georgia counties have a higher rate of prescription opioid-related deaths than the national average.
Mercer Health Sciences Center is uniquely positioned to lead the fight against this deadly epidemic. Central to its mission is preparing healthcare providers committed to the primary care and healthcare needs of rural and medically underserved populations in Georgia.
From the classroom to the bedside, scientists, physicians, physician assistants, pharmacists, physical therapists, nurses and public health professionals are talking with their students, patients and each other about their roles as educators, caregivers and researchers to stem this dangerous tide. All agree much more needs to be done.
One key concern for Jean Sumner, M.D., dean of the Mercer School of Medicine, is lack of understanding of the issues that contribute to the opioid crisis.
“It’s not just doctors overprescribing, not just drug companies making high-powered narcotics. It is a multitude of factors, all of which must be held accountable. It’s communication, education, insurers, regulatory and accreditation agencies. It’s saying ‘Pain is the fifth vital sign,’ a subjective finding that opened the doors to manufacturers promoting the extensive use of opioids for pain relief.
“We spend a lot of time in the classroom talking about professionalism, ethics and quality of care,” she continued. “That means doing what’s right for the patient, but that’s not always what patients want if they’re in pain. I’m in favor of controlling pain, but we must be prudent prescribers of every drug out there and consider alternatives like physical therapy.”
Inexperienced or uniformed physicians are often targets for seekers. “Sometimes it’s hard to say no, and sometimes the unhappy patient goes online and rates the doctor poorly because he didn’t get the drugs he wanted,” Dr. Sumner said. “So it takes well-trained doctors who are confident in their ability, who know their patients and who want to do the best for their patients.
“That’s why we’ve got to re-establish the primary care workforce so every patient has a doctor they can trust to give the best advice and connect them to specialty care they might need. Re-establishing that value is part of solving the opioid crisis, and we’re committed to it at Mercer. We believe when quality and safety increase, overprescribing and inappropriate care goes down.”
The United States has the world’s highest rate of opioid addiction and mortality. Over the past 20 years, the number of opioid prescriptions has quadrupled.
Habitual behavior and addiction
Habits and addiction share common characteristics such as inflexibility and insensitivity to punishment. “For example, addicts will continue to use drugs even though they lost their job, family or have been to jail,” said Ashley Horner, Ph.D., associate professor of pharmacology in the School of Medicine. She studies underlying neural pathways involved in development of habitual behaviors.
The neuropharmacologist has trained rats to habitually consume sucrose and has discovered that removing a tiny sub-region of the basil ganglia in the brain can prevent that habitual behavior. That tiny pathway contributes to inflexible behavior.

With funding from the National Institute on Drug Abuse, she hopes to duplicate those results with drugs of abuse like methamphetamines and opioids. She’s found that blocking mu opioid receptors prevents animals from forming an association between the environment and the rewarding effects of meth. Opiate blockers, such as the overdose-reversal drug naloxone (Narcan®), can treat the repetitive and drug-seeking behaviors associated with meth addiction.
In the classroom, Dr. Horner teaches medical students how drugs affect the brain, as well as risk factors and how to assess whether a patient might need an opioid medication for an injury. Does that patient have a history of mental illness or depression? Are they in a stressful situation or an environment that might make them more susceptible to abusing drugs?
Making sure patients understand the pitfalls of abuse is important as well. “We emphasize the importance of taking medication as directed. Sometimes patients think ‘I’m in a lot of pain, so more medicine must be better so I’ll take two pills instead of one.’ That escalates and soon it becomes four pills and on and on.”
Prescribers need education, too, Dr. Horner stressed, recalling how her mother, age 84, broke her arm and a vertebra in her neck a couple of years ago. “Her physician gave her oxycodone for pain, but at no time did anyone say these are powerful opioids and let’s take a minute to talk about them. It’s a conversation that’s important for physicians to have with patients.”
Mercer is accelerating its efforts to get that message out to providers with prescriptive authority — physicians, physician assistants and nurse practitioners. A Primary Care Update event presented by the School of Medicine, College of Nursing and Northside Hospital this fall drew 80 physicians and nurses to hear the perspectives of a psychiatrist, a pharmacist and a physical therapist. Dozens of physician assistants attended a seminar on “Addressing the Opioid Addiction Epidemic,” hosted by the Department of Physician Assistant Studies in the College of Health Professions during the same weekend in October.
One of the presenters, Jennifer Elliott, Pharm.D., clinical assistant professor of pharmacy practice, teaches Mercer students about the role of pharmacists in understanding patients’ pain, as well as appropriate doses and formulations for pain, how to taper patients off opioids and how pharmacists can help deal with opioid overdoses.
Her students often ask about the legal aspects of opioid dispensing — what they should and shouldn’t do, what they should fill, how to send away a patient effectively. “Pharmacies being robbed for opioids by desperate patients is the No. 1 worry,” Dr. Elliott said.
Opioid-related deaths in this state have increased more than tenfold over the past 15 years compared to a fourfold increase across the rest of the nation.
Georgia laws respond to epidemic
Dr. Elliott also is a clinical pharmacist at Grady Hospital where she sees many patients seeking pain medicine. She now has access to the state’s Prescription Drug Monitoring Program (PDMP), an electronic database that provides prescribers and pharmacists with patients’ controlled substance prescription history and protects patients at risk of abuse. Georgia is one of 11 states covered by the PDMP.
Another new law in Georgia allows anyone who has abused opioids or thinks a family member is at risk of overdosing to get the overdose-reversal drug Narcan®. Mercer pharmacy faculty like Dr. Elliott and Robyn Lorys, Pharm.D., clinical assistant professor and director of the Clinical Skills and Simulation Laboratory in the College of Pharmacy, teach Mercer’s future pharmacists, homeless people and Narcotics Anonymous participants how to administer the life-saving agent.
The pros and cons of the Georgia law providing standing orders for Narcan® stir debate in the substance abuse elective course taught by Katelynn Mayberry, Pharm.D., clinical assistant professor of pharmacy practice. Does this standing order provide a solution to the addiction problem? Should insurance be required to cover services that treat substance abuse?
Dr. Mayberry, whose specialty is psychiatric pharmacotherapy, approaches substance abuse from a mental health perspective, including depression, anxiety and bipolar disorders. Her students are required to attend an NA or AA session to help humanize their perception of those with substance abuse disorders.
She recognizes progress in tackling the opioid epidemic, but worries about other trends. On the positive side, “Thanks to Georgia’s 911 Amnesty Law, if you see someone overdosing, you can call 911 and you and the victim won’t be prosecuted for possession of controlled substances.” On the other hand, she and Dr. Lorys are deeply concerned about the direct role consumer advertisements play in the epidemic.
“You watch TV and see these drugs advertised, and while you don’t even know what the drug is, you feel a simple solution can be achieved by taking a pill,” Dr. Lorys said.
A pill for a pill?
A clinical pharmacist for 26 years, Dr. Lorys contends working with a pharmacist can make a difference in this epidemic. “There are several key factors that pharmacists can address, including patient counseling, assessing patients for substance use disorder risk and appropriate intervention with providers as needed.”
Working with students taking research electives, Dr. Lorys studies outcomes of medication-assisted treatment and what factors put people at risk for addiction. She helped develop a survey directed to pharmacists on the use of the PDMP and subsequent interventions with other healthcare providers. Using the survey, Dr. Lorys hopes to enhance pharmacists’ intervention to help curb opioid addiction.

Dr. Murnane, a pharmacologist, takes another approach. “No matter how much some physicians, pharmacists and drug manufacturers are able to change their practices, or how much we destigmatize the disease, opioids will continue to be dangerous drugs,” he stressed. “We need better drugs for pain.”
With funding from a Georgia Research Alliance grant, he and Department of Pharmaceutical Sciences colleagues are developing drug delivery systems to treat ADHD and cocaine-use disorder that minimize their abuse potentials. Another grant from the National Institute on Drug Abuse underwrites the search for a better understanding of another class of dangerous drugs called cathinones (more commonly known as “bath salts”), which also have been associated with a growing number of drug overdoses.
Ajay Banga, Ph.D., professor and chair of the Department of Pharmaceutical Sciences, is driving a project to develop a patch for children who have oral surgeries each year, in particular tonsillectomies, and can’t swallow well after surgery. In the past, patients would be given codeine for pain, which is synthesized from the opiate morphine. However, a small number of children metabolized the codeine quickly back to morphine and died of respiratory depression.
“We’re trying to make a transdermal patch that will bypass metabolic pathways for morphine,” said Dr. Murnane. Preliminary research shows promise for a similar patch with adult dosing.
Mercer’s College of Pharmacy is the only pharmacy school in the country with its own clinical trial center, a 7,000-square-foot facility that facilitates phase 1-4 studies. Once human trials begin, patches for adults and children could be available within the next five to 10 years, said Dr. Murnane.
Some pharmacy students also are taking action to stem the epidemic. Through the student chapters of the American College of Clinical Pharmacy, they are working with Mercer Police on a drop-off program for unused prescribed medications. These same students can be seen in the state legislature advocating for changes in the law to allow pharmacies to do partial fills.
Promoting alternatives to painkillers
Combatting pain with therapies other than opioids resonates with Timothy McMahon, PT, DPT, FAAOMPT, CertSMT, clinical assistant professor and director of Mercer’s Physical Therapy Clinic, as well as Ruth McCaffrey, DNP, ARNP, FNP-BC, GNP-BC, FAAN, professor and coordinator of the Doctor of Nursing Practice program.
“People want a silver bullet — a pill that’s not addictive and makes pain go away completely. We’re not there yet,” noted Dr. McMahon. “Statistics show that when a physical therapist is involved in patient care earlier in the intervention, the number of patients who go from an acute to chronic pain situation is reduced.”
In Mercer’s Department of Physical Therapy, pain sciences and clinical reasoning are threaded throughout the entire curriculum, including residency programs in orthopedics and neurology. Students learn that patients with structural problems related to overuse or trauma may require some early medication.
“After two to three months, injured tissues usually are in a maturation phase of healing, and inflammation is much less an issue,” Dr. McMahon said. “Patients with persistent pain have likely maladapted to the sustained pain state. Often, a patient with chronic pain has had interpretation changes in the brain, and pain medications and anti-inflammatory medications have little effect.”
Physical therapists today often take a biopsychosocial approach to a patient’s perception of pain versus a pathological anatomical approach, according to Dr. McMahon.
“For example, a patient who has been physically or sexually abused, or has lived in a war zone or an area of strife, tends to have more severe pain and be more prone to chronic pain,” Dr. McMahon explained. “Influences within the brain change a person’s perception of pain.
“Prolonged use of opioid medication has two potential effects on a patient’s central nervous system — the first is the brain turning down pain messages and the second is an activation of immune cells in the brain to make the pain messaging system more efficient. The end result is a heightened sensitivity that requires less stimulus for a patient to experience pain even with plenty of pain medications on board.”
It is common for patients with chronic pain to have anxiety and fear. “We’re trying to educate patients that hurt doesn’t always equal harm. That is especially true with chronic pain. So we try to understand how patients’ stories affect their lives functionally, emotionally and socially, and we help patients retrain the brain through graded motor imagery, pain education and a variety of movement strategies.”
Yoga and other types of exercise also may be effective in managing pain. Dr. McCaffrey in the College of Nursing researches movement therapies for older adults who can’t do standing exercises. An eight-week pilot study funded by Mercer at Decatur Christian Towers compares yoga and a National Institutes of Aging chair exercise program to determine if they reduce pain that interferes with the lives of the participants, ages 80 to 101.
In pharmacology classes for nurse practitioner students, Dr. McCaffrey reviews CDC guidelines that call for non-opioid therapies, if possible, such as physical therapy, massage, heat and cold, or using short-acting opioids for a short amount of time unless the pain is related to end-stage cancer.
Her colleague, Tammy Barbé, Ph.D., RN, CNE, assistant professor of nursing, brings her background in critical care to the classroom. “In an acute-care setting, nurses are with patients more than any other providers,” she said, “and patients feel comfortable talking with nurses. So nurses must be educated holistically to pick up on the subtleties of opioid misuse and abuse.”
An advocate for interprofessional education, Dr. Barbé recently partnered with faculty from the University of North Texas Health Science Center on an Institute for Patient Safety seed grant as its nursing expert in a study examining current practices in pain education within pharmacy, nursing and medical schools.
The U.S. represents less than 5 percent of the world’s population but takes more than 99 percent of prescribed hydrocodone. Opioid overdoses are the No. 1 cause of premature deaths of males. Opioid addiction is the No. 1 reason for incarceration.
Training for the treatment of addiction
Jill Mattingly, DHSc, MMSc, PA-C, clinical assistant professor and chair of physician assistant studies at Mercer, previously worked in addiction medicine and remembers when opioid addiction started to take off in the late 1990s with the marketing of OxyContin®.
What drew her to that field was “seeing that people were struggling with a disease process that was being treated like diabetes was 50 years ago when you were expected to pull yourself up by the bootstraps and stop eating sugar. It’s the same thing with addiction. Organizations like NA and AA do a great job, but often are not enough to treat a disease process.”
Addiction to pain medication has turned into a tsunami that demands many approaches, including medication-assisted treatment, cognitive behavioral therapy, group therapy, exercise, nutrition, and physical therapy.
Since coming to Mercer in 2009, Dr. Mattingly’s goal has been to put significant addiction training into the physician assistant curriculum. “It’s absolutely necessary that all providers be well-trained in treatment of this disease,” she said.
To address addiction, especially in rural and underserved areas, she and colleagues Sheena D. Brown-Waller, Ph.D., MSCR, clinical assistant professor of physician assistant studies, and Tia Solh, MSPAS, PA-C, clinical assistant professor of physician assistant studies, received a $62,500 Health Resources and Services Administration (HRSA) grant in 2017 to teach students, alumni, faculty, preceptors and primary care providers about opioid addiction, diagnosis, prevention and medication-assisted treatment. The latter provides information on how to treat opioid addiction with non-addictive drugs, such as buprenorphine, to reduce craving for opioids. The grant funds one-week addiction medicine rotations at substance abuse treatment centers.
Dr. Mattingly also is taking MAT training national. Under the auspices of the American Society of Addiction Medicine, she teams with Paul Seale, M.D., professor in the Mercer School of Medicine, to present the fundamentals of addiction medicine to PAs, physicians and nurse practitioners across the country.
Dr. Brown-Waller’s research looks at health disparities, like hypertension and addiction, that disproportionally affect underserved populations, and ways to reduce the gap between those who are underserved and those who are not. She attributes the high rates of opioid addiction and death in rural areas to lack of access to care and a high rate of opioid prescribing. Mercer’s PA department received a $1.6 million HRSA grant to train future physician assistants who are from rural areas, or are minorities or veterans, and are interested in practicing in underserved, rural areas to help alleviate the access gap.

Needed: Public awareness
Nannette Turner, Ph.D., MPH, associate professor and chair of the Department of Public Health in the College of Health Professions, said the greatest effect of President Donald Trump’s recent declaration calling the opioid crisis a “public health emergency” is raising awareness. Like many of her colleagues across the Mercer Health Sciences Center, she hopes that funding for new research, education and other public outreach will follow.
Dr. Turner’s longtime interest in addictive behavior has evolved as trends in America have changed. “Tobacco was the big concern 10 to 15 years ago, but now opioid abuse has gone mainstream. Tobacco addiction is more chronic — as smokers age, you see the bad effects of that habit.
“Opioids, on the other hand, are synthetic and more potent. The trajectory to death is shorter. People are dying from opioids at an alarming rate, and we’re seeing more students who want to work in public health capacities that address addiction.”
For example, a current second-year public health student is interning with the Georgia Department of Public Health’s Opioid and Prescription Drug Project, which is developing a statewide response to the opioid crisis.
Mercer’s public health faculty are gathering data about opioid addiction in Georgia, particularly in the northwest and southwest corners of the state, which have the highest incidences of opioid abuse. “If you are in a rural community, you may be doing work that could make you more prone to injuries, and, in turn, you may seek pain relief that could lead to addiction and could be exacerbated by lack of treatment facilities,” Dr. Turner said.
Exploring alternatives to opioids, such as physical therapy and counseling, is at the heart of this research, along with approaches like educating providers, preventing injuries in the workplace and addressing social determinants such as poverty and joblessness that lead to despair and drug seeking. Dr. Turner expects to propose more emphasis on communication using social media and other technologies to counter the epidemic — for instance, using telehealth to provide mental health services like counseling to patients in pain or battling addiction.
“It’s a gargantuan task,” she said. “We are trying to add to the knowledge base and find solutions that could be implemented on a large, population-based scale.”
In the meantime, opioid addiction and opioid overdosing promise to worsen, she said.
“Businesses are finding it difficult to fill jobs because so many people test positive for opioids. It’s starting to affect people financially, and, when the bottom line is affected, people at the national level start getting upset. I’m glad the state is looking at it, but academic institutions need to get involved, too. We certainly are doing so.”