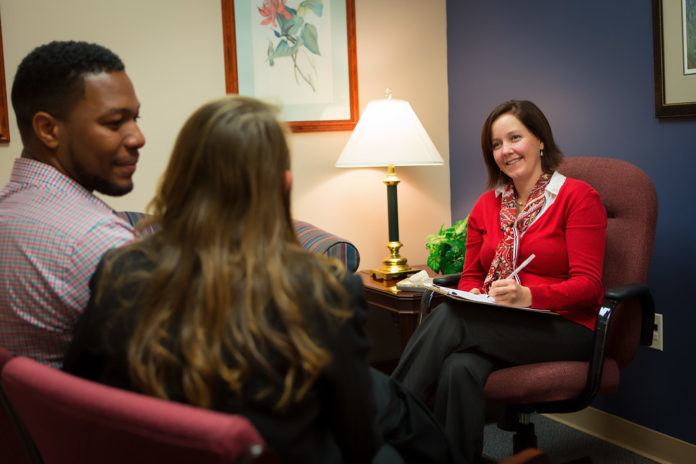The Mercer Family Therapy Center is closed for in-person visits, but patients continue to receive the services they need through telehealth.
Students in the Master of Family Therapy program at Mercer University’s School of Medicine have been providing telehealth services since April, when Georgia Gov. Brian Kemp issued a statewide shelter-in-place order in an effort to reduce the spread of COVID-19.
“Many clients are experiencing higher levels of stress and anxiety, which can exacerbate struggles that were present before the pandemic,” said Dr. Andrea Meyer Stinson, associate director of the M.F.T. program. “During this time, families are also under increased stress due to financial strain, work/school/life balance, isolation and increased conflict at home.
“By providing telehealth services, we can address these stressors and potentially reduce the negative impact of COVID-19 on our clients and community members.”
Students are providing telehealth services at Mercer Family Therapy Center clinics in Macon and Atlanta, as well as many of the M.F.T. program’s 23 community placement sites. The sessions take place over telephone or a HIPAA-compliant video/audio system.

“My experience in providing telehealth has been incredibly rewarding,” said Julieta Flores, a second-year M.F.T. student who is serving the Children’s Health Center and Crescent House in Macon. “I love that I am able to still work with my clients and provide a space for them to feel safe, vulnerable, empathized with and cared for.”
Breaking new ground
This is the first time the Mercer Family Therapy Center has offered telemental health services.
Students were required to attend a six-hour continuing education training session on the best practices and ethics of telemental health, review best practices from the American Association for Marriage and Family Therapy and watch a one-hour training video, Dr. Meyer Stinson said. Faculty also had to do six hours of telehealth and three hours of tele-supervision training to assist the students in the transition.
In addition, in October, before the pandemic, student therapists attended a two-day workshop hosted by Dr. Benjamin Caldwell, a nationally recognized expert on telehealth services, in Macon.
Since the onset of COVID-19, the Macon clinic has seen some existing clients put therapy on hold because of difficulty finding the time and space for private conversations, said Dr. Andrew Benesh, assistant professor and Macon clinic coordinator. On the other hand, the clinic also has seen more people requesting therapy as they cope with increased stress.
Many clients appreciate the ease of attending telemental health sessions, Dr. Benesh said.
“Telehealth creates unique opportunities to share things like artwork, photographs or other meaningful possessions in therapy,” he said. “Our therapists have also been delighted to meet some of our clients’ pets, who can be an important source of comfort and joy.”
“I love that I am able to still work with my clients and provide a space for them to feel safe, vulnerable, empathized with and cared for.”
Julieta Flores, second-year M.F.T. student
Phone and video sessions create unique challenges, as well, because they change the ways therapists and clients communicate.
“We rely on nonverbal cues — things like eye contact, facial expressions and posture — to communicate our emotions, and these can be harder to convey in telehealth,” Dr. Benesh said.
Because clients are home with their families, it also may be difficult to have an uninterrupted 50-minute therapy session. The therapist sometimes has to be flexible, offering options like shorter sessions or planned breaks to check on kids, he said.
And while technology can sometimes be challenging, say if the client does not have a reliable internet connection, it also can help increase the access to high-quality mental health services to rural and marginalized populations.
“Many individuals and families who live in rural areas or have barriers to attend therapy, such as transportation, childcare, caregiving for adults in the home, can now attend therapy more easily,” Dr. Meyer Stinson said. “This aligns with the mission of the medical school at Mercer: to educate physicians and health professionals to meet the primary care and health care needs of rural and medically underserved areas of Georgia.”
In Macon, the Mercer Family Therapy Center is seeing first responders, medical professionals and other essential workers for free during the COVID-19 crisis. Mercer Medicine, a primary care facility, can provide mental health services for those with insurance.
Equipping students for success
As for the student therapists, they’re learning a new skill that can help them after they leave Mercer.
“Telehealth is a treatment format that is growing in popularity and importance and is a skill set that employers are looking for when they hire new therapists,” Dr. Benesh said. “Learning how to provide telehealth services better equips our students to succeed after graduation and gives them experience working with populations they otherwise might not.”

Kendall Davis, a second-year M.F.T. student serving the Atlanta Medical Center, has been holding telehealth sessions from her home office. She said she’s grateful Mercer has provided the resources and training needed to be certified in telehealth, allowing her to continue to help clients during the pandemic and preparing her for the future.
“This experience will also help me to become a better therapist in the future as I learn how to support my clients from a distance and challenge myself to continue working when I am faced with adversity,” Davis said.
LeTese Council, a second-year M.F.T. student who serves the Family Health Center in Macon, had similar takeaways from the experience.
“It has given me the ability to feel comfortable conducting telehealth sessions, shown me how to do certain things to improve session time and quality, and has prepared me for future sessions when it comes to expressing the importance of mindfulness meditation and its benefits,” Council said.
Flores said providing mental health services during this time has made her feel encouraged and uplifted.
“This is a time for us to come together as a community, and I am incredibly thankful I can do my tiny part in being there for others,” she said.