MACON – Mercer University School of Medicine, Navicent Health, Putnam General Hospital, Georgia Partnership for TeleHealth, Community Healthcare Systems Inc. and around a dozen other organizations recently launched the Hancock County Healthcare Access Initiative in the rural county in east central Georgia.
The initiative, which has received support from officials such as Georgia Gov. Nathan Deal and State Sen. David Lucas, serves as the pilot study for a groundbreaking project involving telehealth, which is the delivery of health-related services and information through telecommunications technologies.
“This initiative will provide a great opportunity for Hancock County as far as economic development, but it will also be the start of a program that we can implement across rural Georgia where health care is desperately needed,” said Sen. Lucas, who represents Georgia's 26th District, which includes Hancock, Washington, Wilkinson and Twiggs counties as well as portions of Bibb, Jones and Houston counties.
“Telehealth is going to be a vital part of any sustainable rural health initiative,” added Jean Sumner, M.D., associate dean for rural health in Mercer's School of Medicine. “Mercer is delighted to be able to lead this effort along with our partner organizations.”
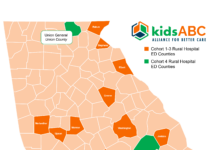
The Hancock County Healthcare Access Initiative is set in an area severely lacking health infrastructure. Hancock has no full-time primary care physician, and residents often seek help 25 or more miles away at one of the area's hospital emergency rooms. Some 68 percent of the calls to 911 are not emergencies, but they often tie up the county's sole ambulance service.
“Georgia Partnership for TeleHealth is excited to see this telemedicine initiative come to life in Hancock County. This program will become a model for the nation as other states struggle with the problem of getting health care to areas where access is often difficult. As care becomes more patient-centered, it only makes sense to provide healthcare access where the patient is – in the home,” said Sherrie Williams, executive director of Georgia Partnership for TeleHealth.
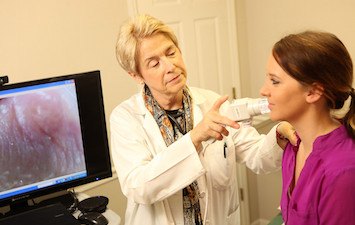
Earlier this month, Excelsior Ambulance Service in Hancock County first employed a telehealth unit – including a high-resolution camera, stethoscope, EKG machine, basic lab equipment and a tablet computer – while responding to a call. Emergency medical technicians are trained to use these units to allow doctors working at partner hospitals to remotely examine and treat a patient and decide if he or she needs to be transported to one of these hospitals.
For the Hancock County initiative, EMTs who are trained in the use of the equipment as well as physical examination skills use the telehealth units to communicate with physicians at Putnam General and Navicent Health, who provide the patient consults.
“Emergency Department physicians and board leadership at Putnam General Hospital are behind the Hancock County Healthcare Access Initiative 100 percent,” said Alan Horton, FACHE, administrator at Putnam General Hospital. “Putnam General is committed to improving access to care in rural Georgia. If our physicians can examine and recommend treatment for patients remotely, then potentially life-saving emergency personnel can remain in Hancock County to be more readily available to respond to emergency situations.”
The project's partners believe telehealth offers a better way to save lives, time and money. They include Mercer, Navicent, Putnam General, Georgia Partnership for TeleHealth, Community Health Care Systems, Stratus Healthcare, the Hancock County Board of Commissioners, Sparta city leaders, the Georgia State Office of Rural Health, Department of Community Health, Department of Public Health, Emergency Management and Prevention, Verizon, AT&T, Roche Diagnostics and more. The Department of Public Health in Mercer's College of Health Professions plans to help publish the costs, outcomes and satisfaction of the project. Additionally, on Sept. 6, Grady EMS will succeed Excelsior as Hancock County's ambulance provider.
“I am proud that Hancock County was selected for this pilot project,” said Hancock County Commission Chair Sistie Hudson. “Our county's healthcare needs will be greatly enhanced through telehealth technology, as non-emergency calls can be handled without unnecessary trips to our neighboring hospitals. It is a win-win for everyone.”
The goal of the Hancock County Healthcare Access Initiative is twofold – first, to build the primary health infrastructure in Hancock County, and second, to develop a telehealth-based business model that's sustainable.
Eventually, the approach may be replicated statewide. Subsequent phases that are planned for the project include elective home visits, post-hospital visits to make sure patients understand their discharge instructions and medications, and elective visits paid by credit card or cash for anyone who doesn't know a physician or doesn't want to make a trip to the doctor.
“Community Health Care Systems has been able to utilize this system to treat homebound patients by having an EMT present the patient to the provider in the Sparta office. Using the peripheral devices, the provider was able to conduct a face-to-face visit with the patient that provided the same information that would have been received if the patient had been in the office,” said Carla Belcher, CEO of Community Health Care Systems Inc.
“Working with the EMT, the patient had a complete assessment without leaving the home. We believe this type of intervention can greatly enhance our access to patients that are homebound or have other transportation barriers that prevent them from being able to come in for a traditional office visit.”
About the Mercer University School of Medicine (Macon, Savannah and Columbus)
Mercer University's School of Medicine was established in 1982 to educate physicians and health professionals to meet the primary care and health care needs of rural and medically underserved areas of Georgia. Today, more than 60 percent of graduates currently practice in the state of Georgia, and of those, more than 80 percent are practicing in rural or medically underserved areas of Georgia. Mercer medical students benefit from a problem-based medical education program that provides early patient care experiences. Such an academic environment fosters the early development of clinical problem-solving and instills in each student an awareness of the place of the basic medical sciences in medical practice. The School opened a full four-year campus in Savannah in 2008 at Memorial University Medical Center. In 2012, the School began offering clinical education for third- and fourth-year medical students in Columbus. Following their second year, students participate in core clinical clerkships at the School's primary teaching hospitals: Medical Center, Navicent Health in Macon; Memorial University Medical Center in Savannah; and The Medical Center and St. Francis Hospital in Columbus. The School also offers master's degrees in family therapy, preclinical sciences and biomedical sciences and a Ph.D. and Psy.D. in clinical medical psychology.