By Rev. Ryan K. Yaun
It was a high-excitement day. We were at the OB's office to learn the gender of our child we were awaiting. The ultrasound tech did her usual checks for all body parts that should be developing. We learned we were having a boy, and we were going to call him Hollis. And then the room changed. I saw the puzzled look on the face of the ultrasound tech. She looked like someone who had some bad news. She calmly set down her equipment, and said that she wanted to get some help reading the ultrasound.
We then learned that Hollis had a condition known as Congenital Diaphragmatic Hernia (CDH). I learned that most of us have a diaphragm that separates our lower abdominal organs from the organs in our chest. Hollis had a hole in his diaphragm. His intestines, stomach, spleen, and part of his liver, had passed through that hole and were located up in his chest. Surgically repositioning all his organs to where they belong after he is born is not such a big deal. The critical issue is that he will have at least one severely underdeveloped lung as it cannot grow without the space to grow, and possibly heart issues.
So, after a few months of appointments with doctors in Birmingham for high-risk situations, we developed a plan. That plan went haywire when Hollis arrived a day before his scheduled induction. Kelly and I got to be with him briefly. Within an hour, he was on a helicopter to Birmingham. And we didn't know if that might be our last time with him. I drove to Birmingham to be with Hollis, leaving Kelly behind in Montgomery.
Hollis was evaluated upon arrival at Children's Hospital in Birmingham. After reviewing his condition, and learning that he also had significant heart defects in addition to his CDH, his Dr. told me Hollis had less than a 20% chance of survival.
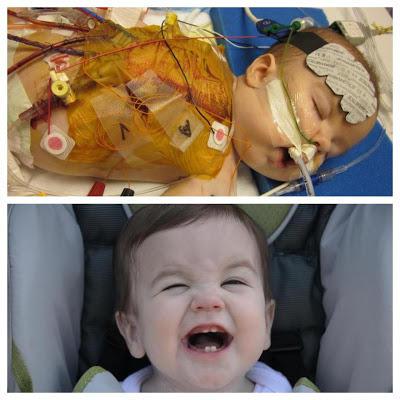
On day 2, Kelly arrived to join me in Birmingham. At 3am, my phone rang. It was the NICU calling. “Hollis is coding. You need to come up here.” We gathered our wits as quickly as we could, and made the short drive to the hospital from the apartment we were using. After coding for 20-30 minutes, they got him back. Later that day, Hollis would be placed on ECMO, a heart/lung bypass machine. This would keep him alive for a brief span of days. If something went wrong, there were no next steps. After 7 days, he came off ECMO. He had his diaphragm repaired at 13 days old. He was taken off the ventilator on Christmas Day, just shy of a month old. He would remain in the NICU until he was 2 months old. We would go home, with Hollis on home oxygen, and return when he just wasn't doing great at home. At 3 months old, he had open-heart surgery to repair his multiple defects. This coming November, Hollis will be 2 years old.
I am a hospital chaplain. I've been to plenty of Code situations. I know the statistics of survival. I know the realities of medical improbabilities. I watch as so many people have to say goodbye to their loved ones.
I am a dad. I couldn't believe this was happening. I struggled with my own grief of what was to come. I raged at God for this happening, and begged God for a miracle.
We had tons of support from family and friends, and every ounce was needed. There were people who sent prayers, food, money, encouragement, and concern. Kelly developed the phrase, “Hope for Hollis,” which became the title of the Facebook page we created to keep friends updated. Hope was what I had when my faith was crushed.
I love my son daily, and am thankful for him daily. But, I have also found myself in the world that I didn't see before, the world of parents who have children with difficulties. I am friends now with so many parents who must learn to live, when their children didn't. And it is painful to see this world that was once hidden from me. Right before Hollis was born, and right after I returned to work, I was involved in cases at the hospital where children died. It crushes me everytime. There were little ones who did not survive during our residency in the NICU. And the shockwaves of being so close to death were overpowering.
When things felt worse, I typically snuck off to the chapel of whichever hospital I was in. I didn't go there to pray. I went there to weep and mourn. And while God exists beyond the hospital chapel, I needed my tears to feel sacred. I needed to feel as though God took time to look and take notice. If my tears fell in a sacred place, I had hope that we would know life rather than death. I didn't cry just for my emotional release, but for my faith in God, and in my Hope for Hollis.
As I'm further removed from Hollis's most critical events, I'm finding that I indeed had Hope for Hollis, but I've also gotten so much Hope from Hollis. I've found hope that Love has power, even in the darkest of moments.
In my professional life, I try and practice pastoral care to the best of my ability. I've given up answering the toughest theological questions. Rather, when asked, I just leave them hanging…unanswered. I find the greatest value in presence. I find sacred space by sitting on the tile floor of the hospital, when someone is so paralyzed by their pain and grief that they can't get up from that spot.
In all of my celebration for my son and his life, I am still burdened by my own survivor's guilt, and for all the parents who have learn to manage through the life I only imagined, but feared it would crush me. My faith is different now, with a teetering balance between grief and hope. When I give thanks daily for Hollis, and life given, I remember those who didn't, and don't, survive, and I pray that their parents may find whatever it is in this life to find their Hope again. Like my Hope from Hollis.
Click here to see a video of Hollis.
Rev. Ryan K. Yaun is a 2003 graduate of McAfee School of Theology and currently serves as a chaplain in Montgomery, Alabama.